Bladder cancer: what you need to know
Bladder basics
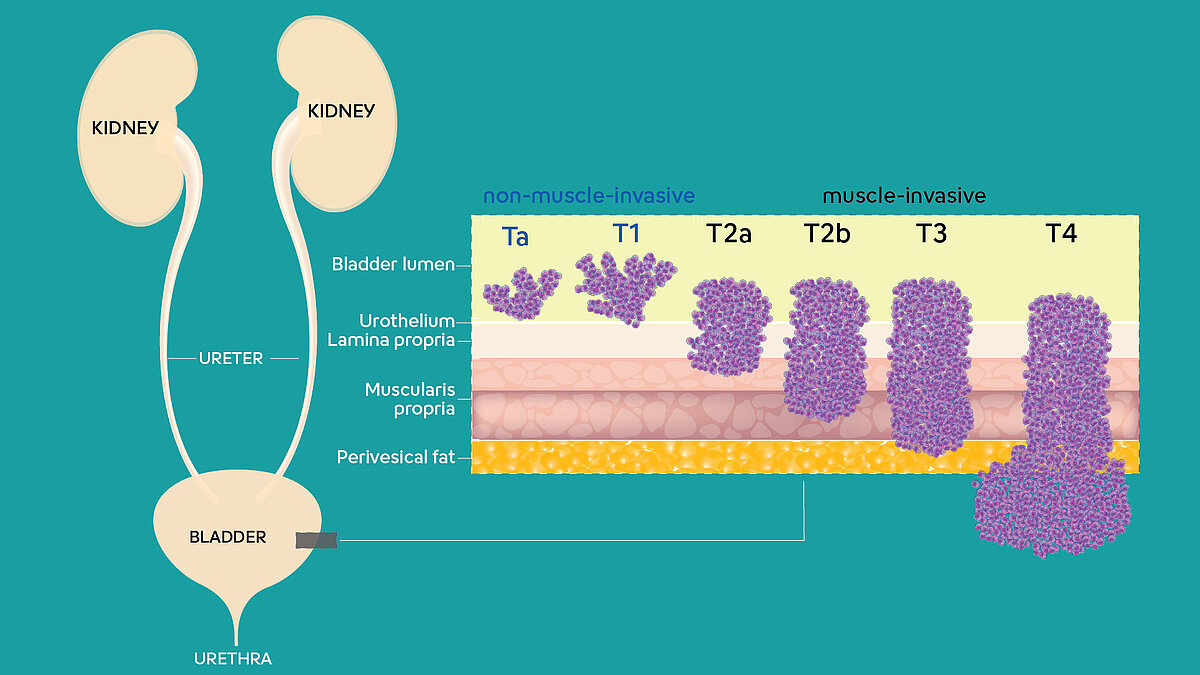
The bladder is an organ in the lower pelvis and has the main job of storing and expelling urine. Urine is liquid waste made by our two kidneys and carried to the bladder through the two ureters. When we urinate, the muscles in the bladder contract and urine is forced out of the bladder through the urethra. A healthy bladder performs this process throughout the day without any hindrances, and we urinate several times a day without issue.
What is bladder cancer?
The wall of the bladder has several layers, with each layer being made up of different kinds of cells. Most bladder cancers start in the innermost lining of the bladder. If cancer develops, it can grow from the innermost lining into or through the other layers in the bladder wall. The more it grows through these other layers, it becomes more advanced and is considered a higher stage, making it increasingly harder to treat. If it continues to grow even past the bladder and into nearby areas, it might spread to nearby lymph nodes or other parts of the body. This is why a clear distinction is made between bladder cancers based on how far they have spread into the wall of the bladder.
Important distinction: invasive vs. non-invasive bladder cancer
Bladder cancer is often further described based on how far it has spread into the wall of the bladder, typically called either invasive or non-invasive. Non-invasive cancers are restricted to the inner layer of cells and have not grown into the deeper layers. These kinds of tumours, as well as any invasive tumours that have not grown into the main muscle layer of the bladder, are also sometimes described as superficial or non-muscle invasive. Invasive cancers have grown into deeper layers of the bladder wall and are more likely spread, as well as harder to treat.
What are causes and risk factors of bladder cancer?
Risk factors for diseases such as cancer can affect your chance of getting it, but are not a guarantee of anything. Different cancers have different risk factors, and some can be changed or improved, while others can’t. For example, living a healthy lifestyle by maintaining a healthy weight and not smoking are things in our control. Whereas age or family history are things we cannot control.
Even though having known risk factors associated with cancer don’t guarantee your fate, it’s still important to be aware of them because you can get things checked out if you notice changes, but you can also lower your risk of getting it. Here are the main risk factors that make a person more likely to develop bladder cancer:
- Smoking: Smoking is the most important risk factor for bladder cancers (and for many other cancers). Smoking causes about half of all bladder cancers.
- Chemical exposure: Certain industrial chemicals have been linked with bladder cancers. Industries carrying higher risks include makers of leather, rubber, textiles and paint products, as well as printing companies.
- Arsenic-contaminated water: In some parts of the world, arsenic in drinking water has been linked with a higher risk of bladder cancer.
- Race and ethnicity: White people are twice as likely to develop bladder cancer than people with other racial backgrounds. The reasons for these differences are not yet understood.
- Age: As with most cancers, the risk of bladder cancer increases with age. Around 90% of people with bladder cancer are older than 55.
- Sex and anatomy: Bladder cancer is much more common in men than in women.
- Chronic bladder irritation and infections: Things that irritate the bladder have been linked to bladder cancer, but it’s not clear if they actually contribute to causing it. Such irritations include urinary infections, kidney and bladder stones, and bladder catheters left in place for a long time.
- Genetics and family history: People who have family members with bladder cancer have a higher risk of getting it themselves. Sometimes family members are exposed to the same cancer-causing chemicals, for example, if members of a family smoke tobacco around each other.
- Chemotherapy or radiation therapy: Even though chemotherapy and radiation are utilised to combat cancer, it can have irritating effects
How is bladder cancer detected and diagnosed?
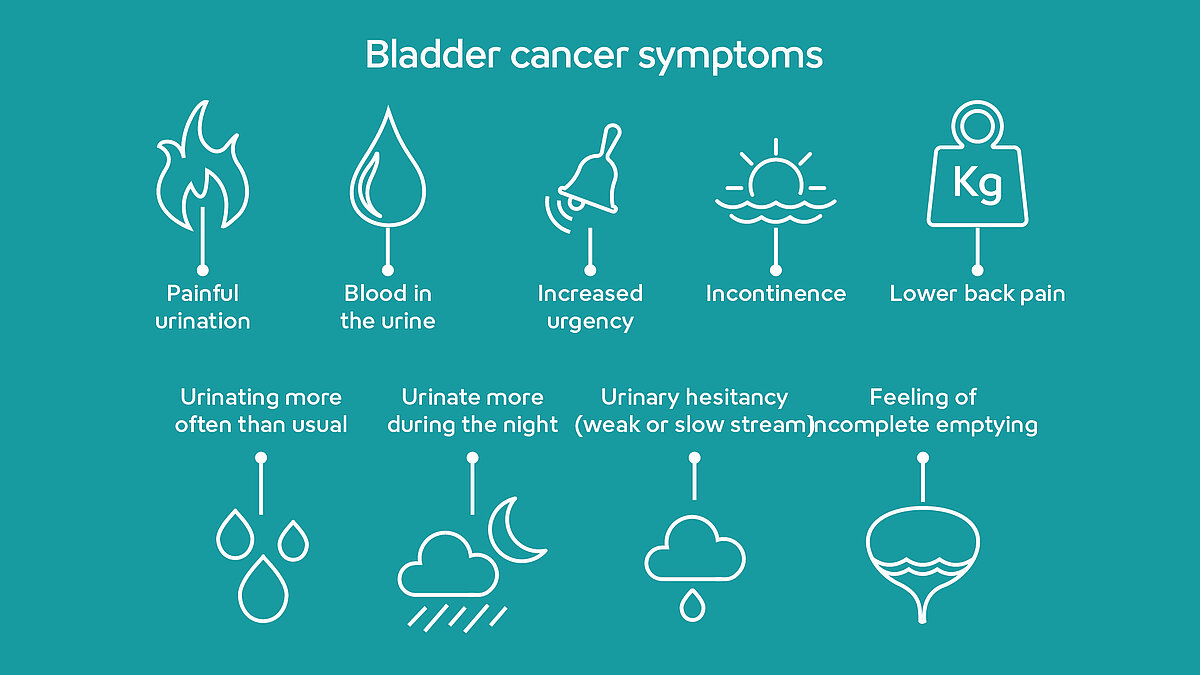
Bladder cancer is typically found because of symptoms a person is having or lab results that are found for a different reason. For example, maybe a patient gets a urinalysis test for other reasons and some abnormal results are found.
At the basic level, a simple urinalysis test can be done to check for blook and other substances in urine. The next step could be a urine cytology test, which takes a sample of urine under a microscope to see if there are any cancer or pre-cancer cells in it. What also may happen is a urine culture, which would be able to rule out if a patient has an infection rather than cancer. Sometimes, urinary tract infections and bladder cancer may cause similar symptoms, so a urine can differentiate that. For a culture, a sample of urine is put into a dish to allow any bacteria that may be present to grow.
If bladder cancer is suspected, most doctors will recommend a cystoscopy, whereby a urologist uses a long, thin, flexible tube with a light and small camera on the end (this is the cystoscope). This is usually done as an outpatient procedure and may take about 10 to 20 minutes to perform, depending on what’s being done. There are other tests that can be performed using dyes and other imaging methods, but cystoscopy is the standard.
If any abnormal areas are seen during a cystoscopy, it will be biopsied to see if it’s cancer. Samples of abnormal-looking tissue are taken and tested for cancer cells. The procedure used to biopsy an abnormal area is a transurethral resection, where the doctor removes the tumour and some of the bladder muscle around the tumour. The samples are then sent to a lab to look for cancer. Testing can also show if cancer has spread into the muscle layer of the bladder wall, which could mean it is at a more advanced stage (non-invasive vs. invasive).

Treatment of bladder cancer
Depending on the stage and other factors, treatment options for people with bladder cancer can include surgery, intravesical therapy, chemotherapy, radiation therapy or immunotherapy. Oftentimes the best option is to include more than one type of therapy.
Surgery
Early-stage bladder cancer tumours can often be removed surgically. The most common kind of surgery for this is called transurethral resection (TUR). A cystoscope is again used for this procedure, but for surgery, a cutting tool is used at the end of it. This cutting tool is used to take out tissues or tumours and heat with be used on the areas around the cut to stop any bleeding. Many people who undergo this surgery can go home the same day, but it depends on how extensive the tumours are.
If the bladder cancer is more advanced, a cystectomy may be performed. With this type of surgery, part of the bladder is removed (partial cystectomy) or all of it (radical cystectomy). If the cancer has spread to the muscle layer of the bladder but it is still small, a partial cystectomy may suffice. However, if the cancer is large and has spread to more than one part of the bladder, the surgeon will likely remove the entire bladder as well as some nearby lymph nodes to check for metastasis.

Intravesical therapy
Intravesical therapy is also used for early-stage cancers and utilises a catheter to inject a liquid medication directly into the bladder. Either immunotherapy or chemotherapy is used. Both therapies work to attack cancer cells, but in slightly different ways, which are discussed based on individual cases with the doctor.
Chemotherapy
Chemotherapy may be administered before any surgical procedures are done. It can help shrink tumours, which makes them easier to remove and makes surgery safer. It also can reduce the risk that the cancer will come back.
This type of therapy may come in pill form or through an IV. Chemotherapy is typically administered in cycles, giving the patient time to recover. Total treatment time may be several months. Chemotherapy may also be recommended after surgery to kill any cancer cells that may remain in the body but are too small to remove.
Radiation therapy
Radiation therapy involves using high-energy radiation to kill cancer cells. It is a more targeted therapy and may require multiple sessions per week for several weeks. It is typically suited for early-stage bladder cancer, patients with early-stage cancer who can’t have surgery, as a follow up to TUR or partial cystectomy, or to prevent or treat symptoms of advanced bladder cancer.
Immunotherapy
Immunotherapy treatment utilises the body’s immune system to attack the cancer. It helps the immune system recognise cancer cells as dangerous and launch a stronger response against them and can shrink tumours or stop them from growing.
Early diagnosis and prevention
There is no definite way to prevent bladder cancer, you should just be aware of the risk factors and do things to lower your risk, especially if you have cancer if your family.
Early detection is also a difficult thing to assess because screening tests are not recommended for people at average risk, such as the case with other types of cancers. For example, urinalysis can help find some bladder cancers early, but it has not been shown to be useful as a routine screening test. Some general health check-ups include a urinalysis, which can find blood in the urine, which can be one of the first signs of bladder cancer (but not always).
Finding cancers early offers the best chance for successful treatment, so as always, it’s important to listen to your body and consult a physician when anything feels unusual.

Sources
[1] American Cancer Society (2022): Bladder Cancer
[2] Treating Bladder Cancer (2022): Treating Bladder Cancer
[3] American Cancer Society (2022): What Is Bladder Cancer?
[4] american Cancer Society (2022): Bladder Cancer Treatments: What to Know